Melatonin and menopause: study says the hormone can help

 Melatonin and menopause, a match made in heaven? A new study by an international group of researchers finds that menopausal women could benefit from taking doses of the sleep hormone melatonin in order to alleviate some of the troubling symptoms of menopause, some of which can lead to further health complications even after the menopausal transition is over.
Melatonin and menopause, a match made in heaven? A new study by an international group of researchers finds that menopausal women could benefit from taking doses of the sleep hormone melatonin in order to alleviate some of the troubling symptoms of menopause, some of which can lead to further health complications even after the menopausal transition is over.
Menopause is the name given to the last stage of a woman’s reproductive age when menstruation ceases to occur (in Canada, the average age of onset is 51) and hormonal changes produce symptoms ranging from hot flashes and night sweats to weight gain, mood disruptions and sleep problems. Insomnia, awakenings in the middle of the night and in the early morning are all common complaints associated with menopause.
And while for a majority of women, these problems dissipate once the menopausal transition is over (which can take years — evidence suggests that women experience symptoms for an average of seven years after the onset of perimenopause), for some, the disturbances of menopause can contribute to more long-term health concerns.
But research suggests that the decrease in production of melatonin could be responsible for menopausal sleep-related issues and thus that supplementation with melatonin doses may help not only with sleep but mood and well-being, too.
Melatonin and menopause: levels decrease with age…
“Melatonin levels decrease (especially at nighttime) with age, particularly during the peri-menopausal period,” say the new study’s authors, an international group of researchers from the United States, Canada, India, Germany and Israel. “This observation has led some to speculate that melatonin may play a role in the menopausal transition.”
Melatonin is a central player in the body’s circadian rhythm, which links up the sleep-wake cycle with the natural day/night cycle. Light turns off the production of melatonin in the body, while darkness causes more melatonin to be produced, which signals the body that it’s time to sleep.
Importantly, melatonin secretion affects the entire body, circulating through to all cells, which means that the impact of having lower levels of melatonin, as experienced in menopause, can be far-reaching, potentially effecting a number of physiological functions.
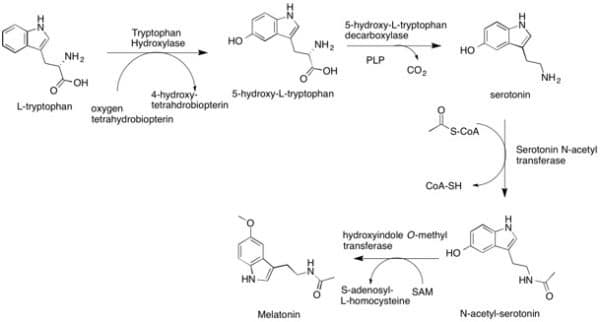
For one, melatonin plays a role in immune system functioning, helping to regulate anti-inflammatory and anti-oxidant responses. “The circadian system controls countless physiological and cell biological functions,” say the authors. “This system exhibits a remarkable complexity.”
To that end, the researchers point to a number of health effects that are a risk to postmenopausal women which studies indicate could be connected to a lack of melatonin, including serious conditions such as depression, fibromyalgia, breast cancer and endometrial cancer. Getting enough melatonin, therefore, through supplements, can help counter the risks of such problems.
“While there is obviously a need for continued research, there are effective behavioural and pharmacological therapies available to treat sleep disturbances at this time in a woman’s life,” say the study’s authors, who suggest that further investigations by randomized controlled studies are “highly desirable” in order to evaluate the efficacy of melatonin-based therapy for peri- and postmenopausal women.
The new study is published in the journal Sleep Science.

