Canadian National Breast Screening Study slammed in new Harvard Medical School article
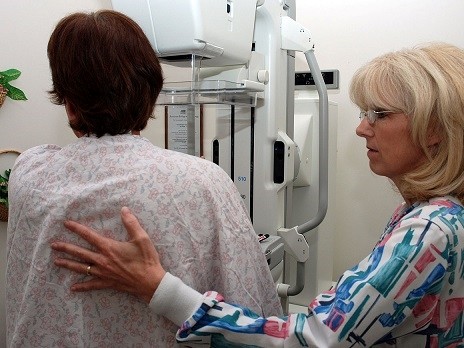
 A new article on the groundbreaking Canadian National Breast Screening Study argues that the study used unscientific methods as well as “poor quality” mammography equipment, both of which effectively compromised the process and rendered the results unreliable.
A new article on the groundbreaking Canadian National Breast Screening Study argues that the study used unscientific methods as well as “poor quality” mammography equipment, both of which effectively compromised the process and rendered the results unreliable.
Penned by Dr. Daniel Kopans of the Breast Imaging Division at Harvard Medical School, the article says contrary to the blind, randomized controlled trials typical of scientific studies, trials for the Canadian National Breast Screening Study (CNBSS), a large five-year study conducted in the early 1980s which contributed to the debate over the efficacy of regular breast cancer screening for women, were “unblinded,” as it was revealed that the women underwent a clinical breast examination prior to participation in the study.
“Women with abnormal clinical breast examinations were identified, and this information was available to the coordinators who then assigned the women on open lists,” says Kopans. “It was, therefore, possible to assign women to whichever arm the coordinator chose.”
Run between 1980 and 1985, the CNBSS involved close to 90,000 women who were assigned to two groups, those who received mammograms and those who did not, with the research intending to shed light on whether or not having mammograms affected rates of breast cancer in women between the ages of 40 and 49.
A follow-up study in 1992 found that after seven years, the rate of death due to breast cancer was not significantly different in the two groups, implying that having regular mammograms did not impact the ability of health care services to detect in time and effectively treat breast cancers.
A further follow-up study published in the British Medical Journal and conducted at the 25-year mark not only confirmed the original study’s results but added the observation that 22 per cent of breast cancers detected during screening of the original study participants turned out to be non-life threatening and were deemed to be cases of over-diagnosing, caused by regular screening.
Kopans contends that because the women were examined before participation in the study, more women with cancers or pre-cancerous tumours were allocated to the screening group, thereby skewing the results.
The CNBSS, which was a first of its kind and has since been described as “probably the most meticulously done randomized trial of screening mammography,” by H. Gilbert Welch of the Dartmouth Institute for Health Policy and Clinical Practice, is said to have influenced health care policy, such as in the United States, where in 2015 the American Cancer Society scaled back its guidelines, now saying that for women without a personal history of breast cancer, regular screening should start at 45 instead of 40. In Canada, new guidelines from the Canadian Task Force on Preventive Health Care do not recommend routine screening for women aged 40 to 49 without a personal history of breast cancer.
Other groups such as the Canadian Association of Radiologists have countered by saying that the evidence supports regular mammography for women in their forties, a position adopted by Kopans. “The scientific evidence clearly supports annual mammography screening beginning at the age of 40,” says Kopans. “The analyses that suggest that screening leads to over-diagnosis of invasive breast cancers are flawed and incorrect.”


