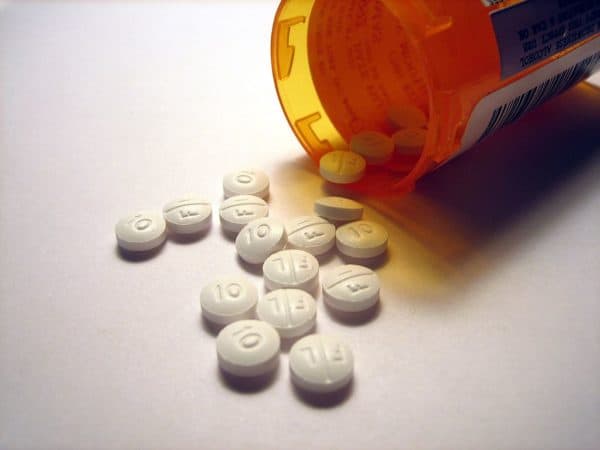
 Opioids and heart disease. It’s not often you hear of the two as a pair.
Opioids and heart disease. It’s not often you hear of the two as a pair.
But a new study from St. Michael’s Hospital in Toronto has found that opioid use in older adults with chronic obstructive pulmonary disorder (COPD) are at a greater risk of heart disease, a potential problem as very commonly opioids are prescribed to adults with COPD.
The study looked at data on over 149,000 Ontario residents aged 66 and older with COPD and found that between 2008 and 2013, 67 per cent of those in long-term care and 60 per cent of those living in the community were given a new opioid prescription for drugs such as codeine, morphine, oxycodone and fentanyl.
The analysis showed that the prescribed opioids were associated with a 215 per cent increase in risk of coronary artery disease-related death for long-term care residents and an 83 per cent increase for community residents with COPD.
“Previous research has shown about 70 percent of older adults with COPD use opioids, which is an incredibly high rate of new use in a population that is potentially more sensitive to narcotics,” said Dr. Nicholas Vozoris, respirologist at St. Michael’s Hospital, in a statement. “Our new findings show there are not only increased risks for coronary artery disease-related death associated with new opioid use, but also increased risk of cardiac-related visits to emergency rooms and hospitalizations.”
Cardiac disease is common for people with COPD, an inflammatory lung disease caused by long-term exposure to irritation of the lungs, most often via cigarette smoke, and can manifest as emphysema and chronic bronchitis. About 20 to 30 per cent of chronic smokers develop COPD, which is also associated with increased risk for lung cancer, contracting respiratory infections and high blood pressure in the lung arteries.
Opiods: heart disease risk is heightened…
COPD can produce symptoms from shortness of breath and persistent cough to swelling in the feet and ankles and chronic muscle and bone pain, and some of these symptoms can be abated through opiate pain medication.
But research on the impact of opioids on heart health is mixed, with some studies showing that they can help protect the heart from blood loss while others suggest that opioids reduce oxygen delivery and increase blood carbon dioxide levels. As well, research has linked prescription opioid use in the general population to increased risk of heart attack and cardiovascular-related mortality.
“It is important for the medical community to be aware of possible opioid-related cardiac adverse events among individuals with COPD,” say the study’s authors, whose research is published in the European Journal of Clinical Pharmacology. “Individuals with COPD may be more vulnerable to potential opioid-related influences on gas exchange given pre-existing impairment in oxygenation and ventilation.”
Between four and ten per cent of Canadians are affected by COPD, with 4.4 per cent of all deaths in Canada in 2011 caused by COPD, according to Statistics Canada. Historically, COPD has had a greater toll on men than women, due to previously higher smoking rates among men.
Although smoking rates for both men and women in Canada have declined since the early 1990s, there has yet to be an associated drop in the COPD death rate, as research has shown there to be a time lag between smoking uptake and death from COPD of about 15 to 20 years in women and 20 to 25 years in men.
Leave a Reply
You must be logged in to post a comment.



 Share
Share Tweet
Tweet Share
Share




Comment