New study says maternal mortality rate exaggerated in the U.S.
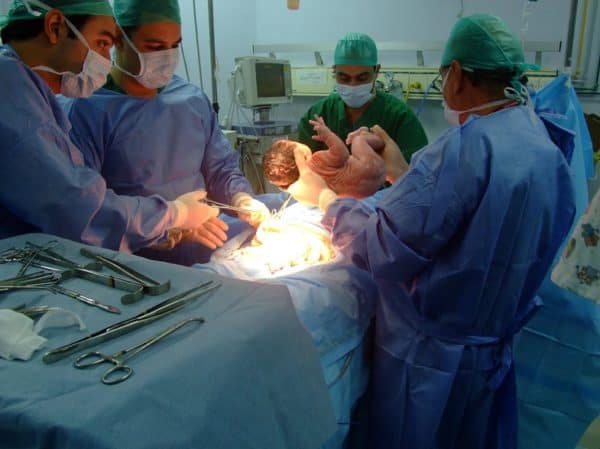
 For some time now, healthcare professionals in the United States have been worrying about an apparent rise in the maternal mortality rate, the death of a woman during childbirth, which recent studies have shown to be steadily on the increase.
For some time now, healthcare professionals in the United States have been worrying about an apparent rise in the maternal mortality rate, the death of a woman during childbirth, which recent studies have shown to be steadily on the increase.
The shock came from studies which detailed a rise in maternal mortality in the U.S. since the late 1980s, where fewer than eight women died for every 100,000 live births, to a high of 18.5 deaths per 100,000 live births by 2013.
What was causing the increase, one which put the maternal mortality rate in the United States higher than that in countries like Azerbaijan, Kazakhstan and Libya? Some blamed bad statistics or the older age at which women were getting pregnant, but many put the blame on poor health. Chronic conditions like obesity, hypertension, diabetes and heart disease are now more prevalent among pregnant mothers in the U.S. than ever before, leading to more dangerous deliveries.
The thought was that all the advances in healthcare and obstetrics over the past century won’t help if the mother is in poor health at the time of birth. Thus, a healthcare emergency was identified and the call to action was put out.
“We must do a better job at addressing maternal mortality in the U.S.” read a 2015 statement from the American College of Obstetricians and Gynecologists. “This means an improved commitment to well-woman care, comprehensive prenatal care and thorough postpartum monitoring.”
While an editorial in the journal Obstetrics and Gynecology, titled “Enough Already!” stated in urgent terms that the medical profession needed to “take ownership” of the society-wide problem by addressing potential causal factors like domestic violence and depression and anxiety, which can play a role in maternal mortality rates. “We can’t make it all better,” read the statement, “but we can do what we do well, only in a more targeted way to meet the patient’s needs.”
But hold on, maybe things aren’t so bad after all.
A new study led by researchers from the Department of Obstetrics and Gynaecology and the School of Population and Public Health at the University of British Columbia in Vancouver found that the apparent rise in maternal deaths over recent decades can be attributed to, on the one hand, improvements in maternal death tracking and better identification of pregnancy status on death certificates, and on the other hand, the adoption of a new international coding system for maternal deaths, one which included previously excluded health complications such as renal disease and other diseases causing deaths which were now being classified as maternal deaths.
Indeed, the study’s authors point to a similar phenomenon in Canada, where vital statistics-based maternal mortality rates doubled following the adoption of new ICD coding, including a 2011 study which identified the rise in maternal mortality as a factor of changes in coding and identifying maternal deaths in Canada rather than a product of a real increase in numbers.
Ultimately, the new study’s authors conclude, while chronic diseases may have amounted to a measurable increase in maternal deaths in the U.S., the problem is far less acute than previously assumed. “The overall picture is not consistent with any serious deterioration in maternal health or maternal health services in the United States,” the authors state.

