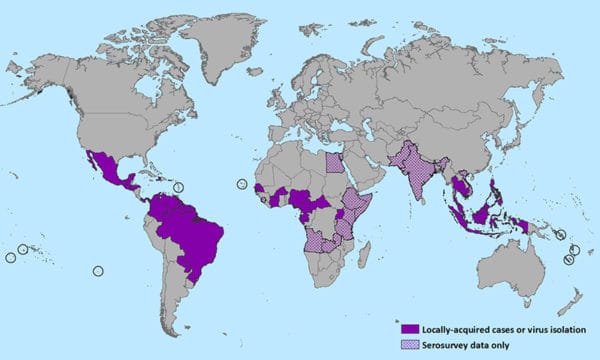

Just as important a question as where the next global pandemics will strike is how quickly will the world’s health authorities be able to coordinate a response.
Bigger than Ebola, more dangerous than Zika, a deadly outbreak of worldwide proportions is expected sometime during the next decade, according to health experts.
The sheer number of new pathogens emerging from previously undisturbed corners of the globe are the threat, with a United States global surveillance group stating that over 1,000 new viruses have been identified from more than 20 countries worldwide.
In August of 2014, the World Health Organization declared the Ebola outbreak in West Africa a Public Health Emergency of International Concern. 11,000 deaths ensued along with related and broader economic, social and health crises.
Assessing the international response to the crisis, a recent report in the British Medical Journal declared that the world remains “grossly underprepared” for pandemic-level outbreaks of infectious disease, saying that glaring deficiencies remain not only in terms of the broader humanitarian response to such crises but also in improving outbreak-related research and knowledge sharing, crucial to fast and operationally-appropriate responses.
“Ebola, and more recently Zika and yellow fever, have demonstrated that we do not yet have a reliable or robust global system for preventing, detecting, and responding to disease outbreaks,” was the dire conclusion of the report.
The quick turnaround in research during periods of infectious epidemics is the focus of a new study led by researchers at the Sunnybrook Health Sciences Centre in Toronto.
Published in the Journal of Critical Care, the study looked at the time taken to complete the necessary start-up procedures for observational research projects on infectious diseases, a critical component to outbreak response and preparedness.
The researchers found that on average it took almost a full year for start-up protocols to be completed, thereby identifying what the researchers see as a major hurdle in infectious disease response.
“This is the first study to report the actual duration of time spent in each step to initiate multisite outbreak-related research,” say the study’s authors. “Our findings indicate that despite an existing in-ICU infrastructure and capability for real-time data collection and reporting, observational research during an outbreak or pandemic is at risk of failing because of the time required for start-up procedures.”
The study looked at time lengths for outbreak surveillance research start-ups at six Canadian intensive care units, covering the various steps involved in research set-up such as average time for receiving research ethics board (REB) approval, average time to execute a data sharing agreement and average time required from receipt of protocol to initiating patient study screening.
The researchers found that the median time to complete start-up procedures was 335 days, noting that the longest stretch of time was devoted to obtaining the interinstitutional legal data sharing agreement, which took on average a full nine months.
The researchers say that too much of the time is wasted in coordinating between institutions (for instance, each institution will have its own fixed meeting dates for REBs) and research start-ups could benefit from greater cross-institutional coordination and parallel reviewing processes specifically dedicated to handling research applications during periods when seasonal or outbreak-related infections are of issue.
“Improving efficiency and parallel administrative activities for certain types of low-risk observational studies are a potential mechanism to mitigate delays in start-up procedures,” say the authors. “Centralized ethics approvals for pandemic research at provincial, state, and national levels may also help to improve efficiency and lessen workload for individual sites.”
Overall, the researchers stress the need for “a nationally and internationally coordinated approach” to meet the observational research needs related to global pandemics, saying that the current, more reactive approach to infectious threats “will likely not allow sufficient time to initiate research before most outbreaks are advanced or completed.”
Leave a Reply
You must be logged in to post a comment.





 Share
Share Tweet
Tweet Share
Share




Comment