 As part of a growing trend in health care called precision or personalized medicine, an international team of researchers has developed an online program, Individualized Lung Function Predictor, for helping patients diagnosed with lung disease.
As part of a growing trend in health care called precision or personalized medicine, an international team of researchers has developed an online program, Individualized Lung Function Predictor, for helping patients diagnosed with lung disease.
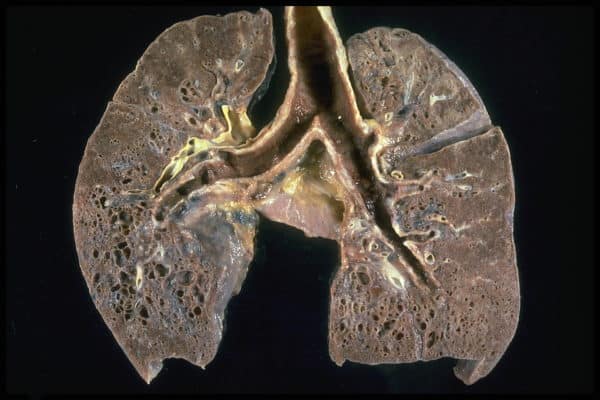
Chronic obstructive pulmonary disease or COPD afflicts 300 million people worldwide as well as one in twenty Canadians over the age of 40. The condition includes chronic bronchitis and emphysema and is caused in the majority of cases by habitual exposure to cigarette smoke, followed by occupational risk factors such as exposure to coal dust and asbestos.
And because COPD is a progressive condition without a known cure, management of symptoms and careful monitoring are all the more crucial for those living with COPD. Yet, up to this point there have been no accurate and effective tests for identifying the disease in its early stages or for gauging the condition’s intensity and activity on an individual basis – hence the value in a new online tool which can help pinpoint the COPD’s progression in each patient.
Developed by a team of researchers including Dr. Don Sin of St. Paul’s Hospital at the University of British Columbia, the online program known as the Individualized Lung Function Predictor allows physicians to input clinical information about each patient and receive a chart predicting the progression of COPD over the coming years, thus helping direct physicians in providing the best treatment options for their patients.
“It sounds simple,” says Dr. Sin, “but it was a complicated research study involving investigators not just here but in the United States and Europe all coming together using a large databases and putting complex mathematical formula to come up with a simple algorithm to determine who has active disease and who does not.”
The work is part of an emerging trend in health care called personalized or precision medicine, grounded in the principle that the manifestations of illness and disease depend greatly on an individual’s physiology, genomic variations and environmental history. Thus, medical intervention and treatment are thought to work best when tailored to the particulars of each person rather than a “one size fits all” model.
A new study shows, for example, that the efficacy of mammogram screening for breast cancer is improved when physicians take into account patient particulars such as age, genetic risk factors and breast density when deciding on screening intervals for patients. Researchers at the University of Wisconsin-Madison Carbone Cancer Center analyzed data on variables such as breast cancer deaths avoided, life-years gained, cost, false-positive mammograms, benign biopsies and overdiagnosis and found that women with average breast cancer risk and low breast density would most benefit from mammograms every three years while women with higher risk and high breast density should be screen yearly.
The individualized medicine movement is “where we need to be at in 2016,” says Sin, whose work is published this month in the Canadian Medical Association Journal.
COPD is the fourth-leading cause of death and the number one cause of hospital admissions in Canada, contributing to more than $2 billion in health care costs.
Leave a Reply
You must be logged in to post a comment.



 Share
Share Tweet
Tweet Share
Share




Comment