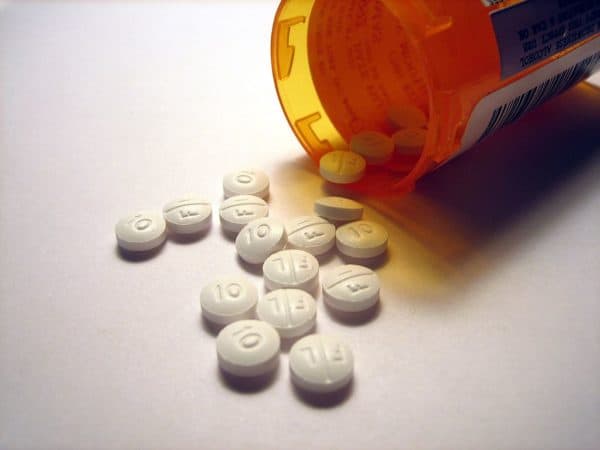
 A pain management and advocacy group in British Columbia is worried that BC’s new guidelines for prescribing opioids could cause more chronic pain sufferers to turn to street drugs for pain medication, a risky prospect according to Pain BC, as pain sufferers can’t be sure of what they’re getting when they buy illegally.
A pain management and advocacy group in British Columbia is worried that BC’s new guidelines for prescribing opioids could cause more chronic pain sufferers to turn to street drugs for pain medication, a risky prospect according to Pain BC, as pain sufferers can’t be sure of what they’re getting when they buy illegally.
“Our fear is that the standards will result in patients being denied access to appropriate options for pain relief and that in turn will drive people to the street-based trade in pain pills,” says the group in a written statement. “An unintended consequence may be an increase in overdoses as desperate pain patients seek medication through illicit sources.”
On June 1st of this year, BC’s College of Physicians and Surgeons instituted a new set of standards for doctors prescribing opioids for pain management, advising doctors to avoid long-term treatment with medications where possible, to prescribe the lowest effective dosages of opioids and to tell patients that alternative approaches to pain management are to be preferred over treatment with drugs.
The change has come about in part due to an acknowledgement by the college of its own role in creating the current opioid crisis -one that saw 371 illicit drug overdose deaths in BC during the first half of 2016, a 75 per cent rise from 2015.
“The public health crisis of prescription drug misuse has developed in part due to the prescribing of physicians,” reads a statement from the college. “The profession has a collective ethical responsibility to mitigate its contribution to the problem of prescription drug misuse, particularly the over-prescribing of opioids, sedatives and stimulants.”
Yet for many pain sufferers, alternatives to medication such as counseling and physiotherapy are not easily accessible, causing many to run out of options. “It’s fine to say to people you need physical therapy, you need some psychological support,” says Maria Hudspith, executive director with Pain BC. “But then, when patients go to find that, they either have no extended health coverage for that or they can’t find a practitioner with the skills in chronic pain in their community. What is available to them is medication.”
The new guidelines are similar in many respects to those issued by the Centres for Disease Control and Prevention in the United States in March of this year, which urged doctors to limit opioid prescription and to offer instead non-opioid painkillers such as ibuprofen and recommend physical therapy. Reaction from pain management advocates in the U.S. echoes that heard in Canada, with some asserting that the new “war on prescriptions drugs” has created a climate of stigmatization for opioid users.
Dr. Jerrold Winter, professor of pharmacology and toxicology at the University of Buffalo worries that chronic pain patients are being “thrown under the bus” by the new guidelines. “I think they go much too far and a) will leave many in pain and b) will drive some seeking pain relief into the illicit market with all its hazards,” says Dr. Winter, who points out that heroin-related death rates in the U.S. have spiked in recent years, a sign that some using prescription opioids may be turning to illicit street drugs in greater numbers. “I fear that this trend will only worsen under the CDC guidelines.”
Comment
Leave a Reply
You must be logged in to post a comment.




 Share
Share Tweet
Tweet Share
Share




What are us chronic pain people supposed to do, just suffer? I have had 3 back surgeries, a handful of times at physical therapy, nerves burnt, and shots in my spine with no relief of pain. I have taken my meds correctly since 2001, never asking for my meds early or running out because I took too many. I live a decent life with medication and can go most of the day with minimal pain. I can’t do things I love like bowl, golf, or anything but I can get around and look like a normal person. Now I am going to suffer in chronic pain, get no sleep, stress 100% of the time and have a horrible life just because I can’t have 1 more pill a day. No one can know what chronic pain is until hey have it. Now limiting our pills is inhumane. No one would let an animal suffer but I guess its ok for a human being to suffer needlessly. You know how stressful it is to suffer knowing you could be helped? I take random drug tests now and always have the right amount of medication in my body. I would do ANYTHING they ask to keep my meds. Take a weekly drug test, have a alcohol monitor machine at home like they do to people with DUI’s. I quit drinking years ago because of my meds and do EVERYTHING right so why do I have to suffer? I am going to try therapy again and try everything possible but if I am still suffering I am going to end my life. I can’t take unbearable pain all day. Who wants to live like that? There are people that have it worse than me, there is going to be massive suicides. I’m only 53, I don’t want to die. I want to enjoy my grandchildren and live normally like I can with pain relief. Druggies are still going to find their fix somewhere. Probably turning to heroin is what most will do. You’re going to have people that never thought of doing that buying heroin now also to help them with their chronic pain. If the meds did cause me to die a few years early I’m fine with that, it should be my choice. At least I lived my remaining years here not in pain and had a far better quality life. God bless all who will be suffering now due to PROP and others.
Occupational therapists enable people with chronic pain to do the things they need and want to do – this includes a variety of daily activities, maintaining employment, and engaging in leisure activities. Unfortunately, in BC access to occupational therapy (OT) services is limited, with wait times frequently reaching 6 to 12 months.
Reduced access to OT and other alternative therapies leads to a reliance on pharmacological treatment, and with the cooling of opioid prescription in BC, there are few options left for those suffering from chronic pain. As recently highlighted by CNN Chief Medical Correspondent Dr. Sanjay Gupta this can result in some unintended consequences, such as an increase in overdose and illicit drug use. We applaud Gupta’s call for doctors to work with their patients to explore alternatives to pharmaceuticals, including occupational therapy. However, without a reallocation of funds to support OT services, it is unlikely that many chronic pain sufferers will be afforded timely access to the benefits that occupational therapists can provide.
Improved funding for OT would mean more options for people with chronic pain, and an addition tool in the toolbox for doctors providing treatment. Occupational therapy services are vital to helping those with chronic pain manage their daily demands, maintain their employment and retain their quality of life, without relying solely on pharmaceuticals.
Giovanna Boniface, OT
Managing Director
Canadian Association of Occupational Therapists- BC Chapter